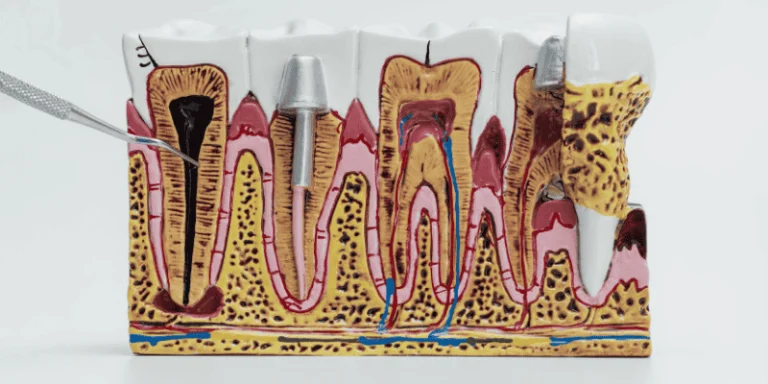
You will get a clear week-by-week picture of what healing feels like after a dental bone graft and what to expect at each step. Most people experience swelling and soreness in the first week, early bone integration over the next few weeks, then steady bone growth and maturation over several months before an implant can be placed.
You will learn simple tips to manage pain, protect the graft, and spot signs that need a dentist’s attention. Expect short changes to diet and activity early on, then gradual return to normal chewing as the graft strengthens.
Key Takeaways
- Healing follows a predictable timeline from immediate recovery to months-long bone growth.
- Proper care and avoiding smoking speed recovery and lower complications.
- Follow-up visits and imaging confirm when the graft is ready for the next step.
Understanding Dental Bone Graft Healing Stages
You will learn what a dental bone graft does, why each healing phase matters, and how the graft becomes a stable base for implants. Expect clear steps, common symptoms, and practical care tips you can use during recovery.
What Is a Dental Bone Graft?
A dental bone graft adds new bone or bone-like material to your jaw where bone is missing or thin. Surgeons may use your own bone, donor bone, animal grafts, or synthetic material to fill the defect. The graft acts as a scaffold that your body replaces with new bone over time.
Right after grafting you’ll have swelling, mild pain, and a clot at the site. Your dentist gives pain medicine and antibiotics if needed, and tells you to eat soft foods and avoid touching the area. Blood vessels grow into the graft in the first weeks, which is key for long-term success.
You should follow care instructions exactly: soft diet, no smoking, gentle oral hygiene, and follow-up X-rays. These steps lower infection risk and help the graft integrate into your jaw.
Why Bone Graft Healing Stages Matter
Each healing stage shows how well the graft integrates and when you can move to the next step, like implant placement. Early stages focus on clot stability and blood vessel growth. Middle stages show new bone forming. Late stages show bone maturing and strengthening.
If healing stalls or you get an infection, the graft can fail. Watching for swelling that gets worse, fever, or persistent pain helps catch problems early. Regular check-ups and X-rays let your dentist track bone density and timing for implants.
Your health also affects timing. Smoking, uncontrolled diabetes, and poor nutrition slow healing. Follow dietary advice, take supplements only if your dentist recommends them, and keep medical conditions under control to improve outcomes.
Foundation for Dental Implants
A successful graft creates enough width and height of bone to hold a dental implant securely. Your dentist measures bone volume with X-rays or a CT scan before placing an implant. Bone must be dense enough to allow the implant to fuse (osseointegrate) with the jaw.
Timing varies. Small grafts may support implants in about 3–4 months. Larger grafts often need 4–6 months or longer. Your dentist will confirm readiness with imaging and clinical checks before drilling for an implant.
During the waiting period, protect the graft by avoiding heavy chewing on that side and keeping mouth care light but thorough. When your jaw is ready, the implant placement is a predictable next step toward a long-lasting replacement tooth.
Types of Bone Graft Materials and Their Impact on Healing
Different graft materials change how fast bone forms, how much new bone you get, and what risks you face. Know which material encourages your own bone growth, which acts mainly as a scaffold, and how each affects infection risk and healing time.

Autograft, Allograft, Xenograft, and Alloplast
Autograft uses your own bone, often from the jaw, chin, or hip. It brings live cells and growth factors, so new bone forms faster and integrates strongly. Expect slightly more pain at the harvest site and a higher short-term recovery need.
Allograft comes from human donors and is processed to remove cells. It lowers surgical time and avoids a second wound. Healing relies on your body to remodel the graft; integration is good but usually slower than autograft.
Xenograft comes from animals (commonly bovine). It mainly provides a mineral scaffold that holds space and guides bone growth. Xenografts keep volume well over months but remodel slowly and may leave residual particles for longer.
Alloplast refers to synthetic materials like calcium phosphate or bioactive glass. These are sterile and predictable, with no disease transfer risk. They act as scaffolds and sometimes release ions that help bone regeneration, but they lack living cells and growth factors.
Bone Graft Material Selection
You should choose material based on defect size, location, and health factors like smoking or diabetes. Small socket preservation often heals well with xenograft or alloplast. Larger ridge defects may benefit from autograft or a mix of autograft plus a scaffold.
If you want fewer surgeries, allograft or alloplast reduce donor-site pain. If rapid, strong integration matters (such as for front-tooth implants) autograft gives the best biology. Ask your surgeon about combining materials; mixes can pair autograft’s cells with xenograft or alloplast’s stable scaffold.
Also discuss healing time: expect 3–6 months before implants in most grafts, but timing can vary by material and site.
Bone Graft Healing Stages: Week-by-Week Timeline
You will see swelling, some pain control needs, and strict care at first. Expect these changes to ease over weeks while new bone starts forming and the graft integrates with your jaw.
Initial Healing (Days 1–7)
You will have the most swelling and pain in the first 48–72 hours. Use prescribed pain relievers and ice packs for 10–20 minutes at a time to control swelling. Keep your head elevated while resting and avoid bending or heavy lifting for the first week.
Bleeding or oozing is common the day of surgery. Bite on gauze as directed and change it only when soaked. Do not rinse vigorously or use straws; these actions can disturb the blood clot.
Stick to a soft-food diet like yogurt, mashed potatoes, and smoothies for the first 7 days. Brush other areas gently and use any prescribed antimicrobial mouth rinse to lower infection risk.
Reduced Discomfort (Week 2)
By week two, swelling should fall and pain will be much lower. You may switch from prescription pain medicine to over-the-counter ibuprofen or acetaminophen, unless your dentist advises otherwise.
Light daily activities are usually fine. Avoid high-impact exercise and smoking, because smoking delays bone graft healing and raises the risk of complications.
You can return to more normal brushing, but avoid the surgical site when cleaning. Your dentist will check the incision and may remove any non-dissolving sutures during this visit.
Progressive Healing (Weeks 3–4)
At weeks three and four you should feel progressively better. Discomfort will be minimal, and the gum tissue will look more healed. Small numb areas or tightness can persist while nerves and soft tissue recover.
New blood vessels grow into the graft during this time, which helps early bone formation. You should still avoid hard or crunchy foods that stress the graft site. Follow any diet timeline your dentist gave you.
Continue follow-up visits and X-rays if recommended. These checks confirm the graft is stable and show early signs of bone integration.
Early Bone Integration (Weeks 4–6)
Between weeks four and six the graft begins integrating with your jaw. Bone cells start to form and replace graft material, a process called early bone integration. This step sets up the longer-term dental bone graft healing timeline.
You can usually expand your diet to softer solids, but avoid chewing directly over the graft until your clinician clears you. Keep up good nutrition; protein, calcium, and vitamin D help early bone formation.
Expect your clinician to schedule imaging around this time to assess healing. If healing looks on track, planning for implants or other restorative steps often begins after this early integration phase.
Long-Term Bone Integration and Maturation
After the first few weeks, the grafted area shifts from soft tissue repair to slow bone rebuilding and strengthening. You can expect new blood vessels to grow in, immature bone to form, and gradual hardening that prepares the site for an implant when imaging shows enough density.
Bone Regeneration and Vascularization (Months 1–2)
During months 1–2, your body replaces the initial clot and graft scaffold with new, soft bone called woven bone. Blood vessels grow into the grafted area to bring oxygen, nutrients, and cells needed for bone formation. This vascularization is critical: without good blood flow, the graft can fail or resorb.
You may feel little to no pain by this stage, though mild tenderness can persist. Keep up gentle oral hygiene and avoid pressure on the site while chewing. Your dentist may take a follow-up X-ray to check early bone fill and the pattern of healing.
Factors that help this phase: good nutrition (protein, calcium, vitamin D), controlled blood sugar, and avoiding smoking. If you have delayed healing or signs of infection (persistent swelling, worsening pain, or drainage) contact your provider right away so they can assess the graft before it progresses.
Bone Maturation and Strengthening (Months 2–4)
From about month 2 to month 4, woven bone gradually converts to stronger, more organized bone known as lamellar bone. This maturation increases density and mechanical strength. New bone thickens and links with your existing jawbone, improving stability at the graft site.
You’ll likely resume most normal activities and a broader diet, but still avoid hard, crunchy foods directly on the graft. Your clinician may use radiographs or a CBCT scan to measure bone volume and density. These images show whether the graft is consolidating or losing height/width.
Factors that slow maturation include smoking, poor oral hygiene, certain medications, and systemic issues like uncontrolled diabetes. If imaging shows inadequate maturation, your clinician may delay implant placement or plan additional grafting.
Osseointegration and Readiness for Implants
Osseointegration refers to the direct biological bond between living bone and a dental implant surface. Before placing an implant, your clinician confirms that the grafted site has enough volume and density to support stable osseointegration.
Timing varies, but many sites are ready between months 3 and 6 depending on graft type and location. Your dentist will check bone quality with clinical exam and imaging, and may perform a bone probe or test implant torque at placement to confirm stability.
Continue following care instructions until the implant is placed. Good bone maturation and vascularization increase the chance that your implant will integrate properly and last long-term.
Factors Affecting Bone Graft Healing and Recovery
Major factors that change how well your bone graft heals include your health, habits, surgical details, and any complications that arise. Small choices like quitting smoking and following care instructions make a big difference to graft success.
Patient Health and Lifestyle
Your medical conditions directly affect bone graft healing. Diabetes, autoimmune disorders, and poor blood flow slow bone formation and raise infection risk. Tell your surgeon about medications, especially steroids or blood thinners, because these can change healing time or require temporary adjustments.
Smoking and vaping cut blood flow and raise graft failure risk. If you stop at least two weeks before surgery and during the first three months after, your odds of success improve. Nutrition matters too: eat protein, calcium, and vitamin D. Stay hydrated and avoid alcohol for several days after surgery to lower bleeding and swelling.
Maintain good oral hygiene without disturbing the graft. Use prescribed mouth rinses and gentle brushing. Attend follow-up visits so your team can spot early problems and act fast.
Complications and Graft Failure
Graft failure happens when the graft doesn’t integrate with your jawbone. Common causes are infection, poor blood supply, mechanical disturbance (like biting hard foods too soon), and smoking. If the graft becomes exposed, you may see pain, swelling, pus, or a bad taste; report this right away.
Infections often show within the first two weeks but can appear later. Your surgeon may use antibiotics, clean the area, or remove graft material if needed. Rarely, nerve damage or sinus problems occur after upper-jaw grafts. Your provider will explain specific risks based on graft size and location.
Watch for warning signs: rising pain after initial improvement, fever, continuous bleeding, or any material showing through the gum. Quick treatment lowers the chance you’ll need repeat surgery.
Optimizing Recovery for Successful Results
Follow your post-op plan closely to protect the graft. Rest for 24–48 hours, use ice for swelling, and keep your head elevated while sleeping. Take pain meds and antibiotics exactly as prescribed. Don’t use straws or spit forcefully; both can disturb blood clots and the graft site.
Diet should be soft and nutrient-dense. Choose smoothies, yogurt, eggs, and soups that are warm, not hot. Gradually reintroduce firmer foods after your provider clears you. Avoid heavy lifting and strenuous exercise for at least one week, or longer if advised.
Keep follow-up appointments and get X-rays when recommended to confirm bone graft healing. If you have questions or notice problems, contact your dental team right away. Their timely checks and your careful home care together lower the risk of graft failure and speed recovery.
Frequently Asked Questions
This section gives direct answers about what you will feel, how healing looks at each stage, what to watch for after two weeks, steps you can take to help the graft heal, typical timing before implants, and clear warning signs of graft failure.
What should patients anticipate during the initial days after a dental bone graft?
Expect swelling, mild to moderate pain, and light oozing for 24–48 hours. Pain usually peaks on day 2 or 3 and improves with prescribed pain meds and ice.
You may see bruises and feel tired as your body uses energy to heal. Keep your head elevated, avoid heavy activity, and eat soft, cool foods.
Follow any antibiotics or mouth rinse your surgeon prescribes. Avoid smoking, alcohol, and using a straw to protect the blood clot.
How can one identify if their bone graft is healing correctly at each stage?
In the first week, look for reduced bleeding, steady but decreasing swelling, and pain that eases with time. A stable blood clot and no fever are good signs.
During weeks 2–6 you should notice less swelling, firmer tissue at the site, and no pus or spreading redness. Your surgeon may confirm progress with clinical checks or X-rays.
From weeks 6–12 and onward, you should feel increasing firmness and return to normal chewing. Imaging should show new bone forming and integration with the existing jawbone.
What are common indicators of a successful bone graft after two weeks?
After two weeks you should have minimal pain and little to no visible swelling. The surgical area should feel more stable when touched gently.
No signs of infection (no fever, no pus, no bad smell) indicate proper healing. Your follow-up visit may show early soft tissue closure and initial bone integration on X-ray.
What steps can be taken to ensure optimal healing of a bone graft?
Take all prescribed medications exactly as directed, including antibiotics and pain relievers. Use cold packs the first 48 hours and start gentle salt-water rinses when recommended.
Eat soft, nutrient-rich foods and avoid smoking or vaping. Keep follow-up appointments and get any recommended X-rays to confirm graft integration.
How long does it usually take for a bone graft to fully integrate before receiving an implant?
Small grafts for a single tooth often need about 3–4 months before implant placement. Medium grafts usually require 4–5 months.
Large grafts or sinus lifts can take 5–6 months or longer. Your surgeon will confirm readiness with clinical exams and imaging before placing an implant.
What are the signs of a failed bone graft that patients should be aware of?
Seek immediate care if you have increasing or severe pain after the first week, persistent fever, or growing swelling. These can signal infection.
Also watch for continuous bleeding beyond 48 hours, exposed graft material, a bad taste or smell, and numbness that does not improve. Any of these signs may mean the graft isn’t integrating and needs evaluation.